Doctoral Internship Program in Clinical Psychology
CHOC, a part of Rady Children’s Health, is pleased to offer four one-year, full time, doctoral internships in clinical psychology, accredited as a doctoral internship in health service psychology by the American Psychological Association. The program is also a member of the Association of Psychology Postdoctoral and Internship Centers (APPIC). The training year begins on August 24, 2026 and ends on August 20, 2027. The internship at CHOC focuses on training advanced level doctoral students in pediatric psychology to work effectively within medical settings with children with acute and chronic medical conditions and their families, as well as offering continued training with more traditional child clinical outpatient presenting problems. All of the training experiences take place within the hospital setting. CHOC is one of relatively few accredited internships which provides year-long specialized training in children with medical diagnoses fully within a hospital setting.
Childhood chronic illness is a significant health concern. As medical treatments improve, more children are living longer with chronic illnesses. It has been estimated that 15 to 18% of children in the US are living with a chronic illness. Of these, about half experience a restriction in their ability to participate in normal activities. Children with chronic illnesses and their families experience a wide range of unique stressors, yet many do not have access to quality mental health services. Uniquely tailored psychological services, such as specialized assessments, psychosocial support, targeted psychotherapy, and consultation with medical teams can have a very positive effect on quality of life for children and their families. In recognition of these positive effects, children’s hospitals and clinics are increasingly working closely with psychologists and other mental health professionals to provide comprehensive services to their patients. The psychology internship at CHOC seeks to train psychologists to work effectively with children with acute and chronic illnesses and their families within the context of hospital- based inpatient and outpatient services, as well as multidisciplinary medical clinics. This is a particularly exciting time to be a part of pediatric psychology as the medical field increasingly understands the critical role of psychological factors in overall health and is thus increasingly involving psychology services into standard health care services. In addition to the intensive experiences with children with medical diagnoses, we believe in offering solid training in child psychology, thus interns also receive training and experiences working with children and families within rotations who do not have a chronic medical condition.
Our past graduates have largely gone on to complete postdoctoral fellowships within a medical setting (over 95% over the past 7 years), with many ultimately practicing within medical settings.
Introduction to CHOC
Children’s Hospital Orange County (CHOC), a part of Rady Children’s Health, serves much of Southern California as it is Orange County’s only medical facility solely devoted to the care of children and their families. Founded in 1964, CHOC is a tertiary care facility with a 334-bed capacity and a medical staff of over 500 physicians. Virtually every pediatric subspecialty is offered here: allergy, cardiology, endocrinology, gastroenterology, hematology, infectious disease, neonatology, nephrology, neurology, oncology, psychiatry, pulmonology, rheumatology and urology. Most surgical specialties are also available. CHOC also has a joint pediatrics residency program with the University of California, Irvine Medical Center. CHOC and the University of California, Irvine Medical School have an affiliation agreement and since 2009, the majority of pediatric care for both facilities takes place at CHOC. In January 2025, Rady Children’s Hospital and CHOC merged to become Rady Children’s Health, with three campuses; Orange County, Mission Viejo, and San Diego. Rady’s Children’s Hospital in San Diego is affiliated with University of California, San Diego Health Science Center. In 2019, CHOC signed an affiliation agreement with PIH Hospital in LA County providing outpatient services and consultation on inpatient cases.
Since opening its doors in 1964, CHOC has provided the highest quality medical care to children. Our regional health system includes two state-of-the-art main hospital facilities in the City of Orange and in San Diego, a hospital-within-a hospital in Mission Viejo (CCMH), and many community clinics in the Southern California area — plus over 100 additional programs and services. With admissions growing by 90% over the last eight years, CHOC and CCMH combined rank as the 15th busiest children’s hospital in the country. CHOC’s transport system ranks among the top three busiest services in the country.
CHOC ranked in U.S. News & World Report’s Best Children’s Hospitals in eight specialty areas: neonatology; cancer; diabetes and endocrinology; neurology and neurosurgery; orthopaedics; pulmonology; urology, and behavioral health with special recognition to orthopedics and diabetes and endocrinology, who ranked in the “top 20” for that specialty. CHOC earned the Gold Level CAPE Award from the California Council of Excellence, the only children’s hospital in California to ever earn this distinction, and was awarded Magnet designation for a second time, the highest honor bestowed to hospitals for nursing excellence. Recognized for extraordinary commitment to high-quality critical care standards, CHOC is the first children’s hospital in the United States to earn the Beacon Award for Critical Care Excellence and the first to win the award twice. CHOC is one of 90 hospitals – and one of only 9 children’s hospitals – across the nation named to the “2016 Leapfrog Top Hospitals” list, based on results from The Leapfrog Group’s national survey. A record number of 1,324 hospitals participated in the survey this year, which measured performance in patient safety and quality. Specifically, the survey focused on three critical areas of hospital safety and care: how patients fare; resource use; and management structures in place to prevent errors. CHOC is the only children’s hospital in California to make the prestigious list this year.
To better accommodate the growing needs of our community’s children, CHOC built a new state-of-the-art patient care tower which opened in 2013. When the new tower opened, CHOC added pediatric surgical suites and related services, emergency, laboratory, pathology, imaging and radiology services, a dynamic and family-friendly lobby with a design including Disney elements (be sure to stop by and see Turtle Talk), outdoor gardens, a café, Starbucks, a teen activity area, and a family resource center. CHOC’s new Southwest Tower opened in June 2025 housing much of outpatient specialty care services with patient and family friendly spaces throughout.
Facilities: CHOC’s six-story North Tower hospital building, which opened in November 1991, is licensed to provide care for 238 inpatients. More recently, CHOC opened the Southwest Tower, a nine-story, state-of-the-art outpatient facility designed just for patients and their families in June 2025. A specialized Pediatric and Cardiac Intensive Care Unit was opened in October 2007. A new addition to the Neonatal Intensive Care Unit (a very low birth weight unit) and additions to the Oncology Unit (additional beds for adolescents) were opened in 2009. In addition, a new NICU unit was opened in July 2017 which offers private rooms for all families. Our medical stabilization of Eating Disorders program moved to CHOC Children’s Hospital at Mission Hospital in Mission Viejo in February 2019. In April 2018, CHOC opened a state-of-the-art Mental Health Inpatient Center (MHIC). The MHIC has 18 rooms, all private. In addition to these beds, there is an adjacent 3300 square foot outdoor activity area. Children from 3 years of age to their 18th birthday can be treated in the MHIC. As appropriate, parents can spend 24 hours a day on the unit (with only one parent spending the night). The MHIC provides multidisciplinary care with psychiatrists, psychologists, nurses, social workers, child life specialists, art therapy, music therapy and behavior techs. The Center is located on the 3rd floor of CHOC West. The MHIC has served over 1000 patients since its opening. In January 2020, CHOC also opened the Thompson Autism Center. The Thompson Autism Center is dedicated to bringing the latest treatments and resources to the Autism community in Orange County. Through unique programs, children have a centralized place where they can receive early diagnosis, specialized advanced therapy, and the possibility to reach their true potential.
Most hospital administrative offices are on the 2nd floor of the Holmes Tower (South Tower, new tower). Most outpatient visits are scheduled in the CHOC Clinic (Specialty Care) in the CHOC West building. CHOC has many Primary Care clinics throughout Orange County with the largest one on Chapman Ave, about a mile from the main campus. Research laboratories (5th floor) and some physician administrative offices (2nd floor) are also in CHOC West. The rest of the physician administration offices are in the 505 building on the 5th and 12th floors. The Department of Pediatric Psychology is located in the Centrum North building, along with the specialty areas of primary care (i.e., Adolescent Medicine, Abuse follow-up Clinic, GPS (Gender, Puberty and Sexual Development, etc.), and additional CHOC administrative offices. Other medical group outpatient offices (such as Cardiology, Neurosurgery, and Hematology) are located in the St. Joseph’s Cancer Center. The Neurosciences and Urology Outpatient offices are in the 505 building on the 3rd and 1st floor respectively.
Outpatient Care: The hospital’s Ambulatory Care Center, or CHOC Clinic, is a full-service outpatient facility. Each year, the Clinic handles more than 70,000 patient visits — encompassing a wide range of care, from well-baby visits to treatment of major childhood illnesses. Besides general pediatric care, the Clinic offers over 20 specialty clinics for everything from allergies to craniofacial problems, so that children with chronic conditions can receive treatment from teams of specialization on a regular basis. In addition, CHOC runs 5 community-based clinics in outlying towns. Outreach clinics are also held at Hoag Hospital in Newport Beach as well as in Corona and Huntington Beach. Seven community outpatient pediatric practices have joined CHOC since 2016, which cover north, central and south Orange County populations.
Emergency Services: CHOC operates a full-service pediatric emergency department (ED) on the 1st floor of the South Tower (new tower). Our ED sees almost 90,000 visits each year and is a Level II Trauma Center. There is a Mental Health team in the ED (MHES) to evaluate children who present with psychiatric emergencies seven days a week for approximately 16 hours per day.
Transport Services: CHOC operates a pediatric transport service to bring children to the intensive services that can be offered at CHOC. The number of patients transported to CHOC increased by 193 percent since 2000, making ours among the three busiest transport programs in the nation. You will note our newest addition, a CHOC branded helicopter on our Helipad atop the Holmes Tower.
Population Health: A CHOC-Rady’s collaboration was the only children’s focused health care system to receive a CMS grant on the use of population health strategies to increase positive outcomes and reduce costs. CHOC has been working on this project for the past 4 years and continues to develop and grow their population health services and approach. Mental health is closely aligned with population health services. In fact, last year one of our psychologists joined the population health team to focus on developing a consistent transition of care program for children with chronic illnesses. Population health is housed on the same floor as Pediatric Psychology/Mental Health in the Centrum Building.
Mental Health Initiative: In 2014, CHOC undertook a leadership role in a Mental Health Initiative in conjunction with community partners, to develop a pediatric mental health system of care for Orange County. As a part of this initiative, CHOC committed to building an 18-bed inpatient psychiatric mental health inpatient unit that treats children from 3 years to 17 years old. This state-of-the-art Center opened in April 2018 (see above). The Mental Health Inpatient Center (MHIC) is the first inpatient psychiatric hospital in Orange County that includes pediatric beds in many years. We also opened a fully adherent DBT Intensive Outpatient Program (IOP) for adolescents based on the ASPIRE program developed at El Camino Hospital in February 2018, and opened a DBT IOP program for middle schoolers in the summer 2024. Further, we have developed a more intensive triage program in the Emergency Department, Mental Health Emergency Services (MHES) to evaluate the needs of children presenting for psychiatric issues and determine if inpatient treatment is necessary, and link to outpatient care if inpatient care is not required. In September 2015, we opened a County Behavioral Health contract clinic, CHOC CYS Co-occurring Clinic, which provided services to children with both medical and mental health conditions. This is a first of its kind specialty mental health clinic for Orange County Behavioral Health. In August 2018, we opened a County Full Service Partnership Program (FSP), Project HEALTH, to provide intensive outpatient and wrap-around services for children with both medical and mental health conditions. In July 2023, our Co-Occurring Clinic merged with our Project HEALTH FSP and now Project HEALTH provides intensive outpatient wrap-around services in addition to ongoing outpatient therapy services. In January 2020, the Thompson Autism Center opened, with mental health professionals serving as key providers, consultants, and team members. In August 2020, we forged a partnership with Mater Dei Catholic High School to create an innovative program to provide mental health services, wellness and educational programming, and staff training for students, parents, teachers, and administrators within the school community. We are also continuing to further develop our inpatient medical stabilization eating disorders program at CCMH, our young child clinic, and integrated primary care.
The CHOC Psychology Department includes psychologists and neuropsychologists (45 psychologists), licensed social workers and marriage and family therapists, art therapists, personal service coordinators, resource specialists, and administrative staff. In addition, CHOC has a Department of Psychiatry. Other specialists involved in providing care for children include pediatricians, psychiatric nurse practitioners, psychiatric nurses, behavioral technicians, art therapists, child life specialists, nutritionists, speech and language pathologists, physical therapists, and BCBA therapists.
Introduction to the Pediatric Psychology Department
The Department of Pediatric Psychology at CHOC provides comprehensive psychological treatment and assessment services to children and their families. Our team of psychologists attends to the emotional, cognitive, and developmental needs of children and adolescents, including children with acute and chronic medical conditions. Consultation is provided to all inpatient medical services hospital-wide. Psychological and neuropsychological assessment and psychological support and/or therapy occur within inpatient and outpatient settings. The Psychology internship is well integrated within the hospital and is administered in collaboration with other professional training programs in pediatrics, child psychiatry, nursing, social services, and rehabilitation within the hospital. Interns have the opportunity to be involved in a full range of departmental activities. Examples of specific departmental activities are listed below.
Specific Department Activities
- Evaluation and treatment of psychological factors associated with medical illness; including adjustment issues, adherence to prescribed medical regimens, parent-child issues, and staff-patient-family dynamics.
- Psychological/Neurodevelopmental assessment
- Consultation and liaison with physicians, nurses, and other health care professionals
- Assessment of patients at high risk for dangerous behavior
- Consultation to the CHOC emergency department, all medical inpatient units, and CHOC medical outpatient clinics, including on call
- Individual, family, and group psychotherapy
- Child psychiatry services
- School re-entry services, including participation in IEPs as appropriate
- Participation in medical services’ rounds and psychosocial rounds
- Provision of educational rotations and seminars to residents and medical staff members
- Pain management evaluations and treatment services
- Psychological assessments and psychotherapy conducted in Spanish for children and families (for interns who are Spanish speaking)
- Infant, toddler, and preschool development and developmental disabilities evaluation, consultation and treatment
- Working with Pediatrics Residency Program on wellness activities
The Training Program
The doctoral internship in health service psychology training program at CHOC specifically focuses on the development of specialized professional skills in pediatric and child clinical psychology. We expect that interns will enter the program with previous experience in child psychotherapy and child assessment. During the year, interns will receive first-hand experience in applying their knowledge of child development and their skills as a child therapist to children with co-occurring medical and mental health conditions. Interns have the opportunity to do this through a wide variety of experiences, such as inpatient consultation-liaison services to a variety of medical specialty units, more intensive experiences with specific medical specialty teams, and outpatient psychotherapy. In addition, the internship is committed to providing appropriate and relevant services to culturally diverse families. As an intern, you will be exposed to a multicultural context that challenges the professional practice of even the most seasoned psychologists. Orange County offers a very culturally diverse population.
Internship Structure
Interns at CHOC participate in a variety of training activities. Interns have the opportunity to receive both a breadth of experience with children with medical diagnoses and more traditional child psychopathology along with in-depth experiences with specific specialty medical teams. There are a variety of core training experiences that take place throughout the entire training year. Trainees participate in two six-month specialty rotations through an array of CHOC specialty services and clinics. Each training experience is described below.
While time spent in each activity can differ on a week to week basis, the basic breakdown of time spent in each activity is as follows (chart based on 40 hour week):
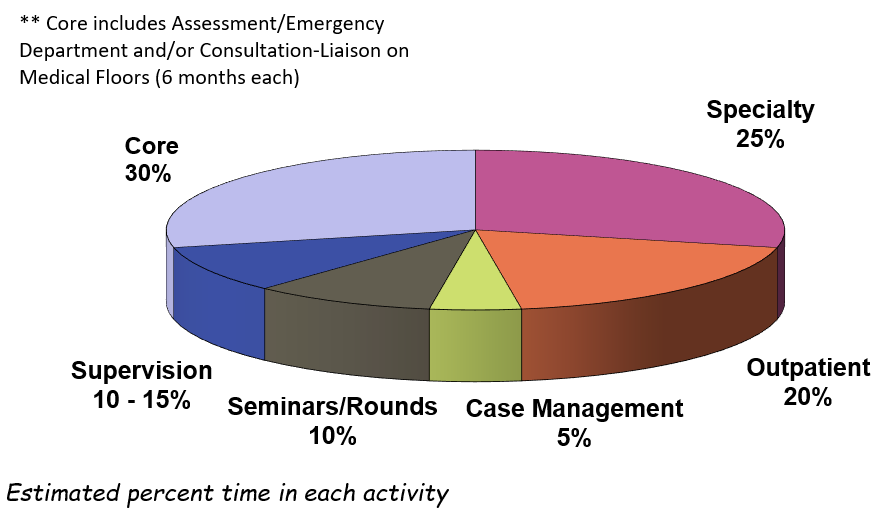
Core Rotations
Outpatient Therapy Rotation (12-month rotation): Interns will participate in CHOC Psychology’s Medical Coping Clinic (MCC) as their outpatient therapy and diagnostic evaluation experience for the full 12-months. Medical Coping Clinic provides short-term therapy (4-16 sessions) to patients ages 8-18 who are experiencing an overlap between their medical conditions and mental health functioning. This rotation offers an opportunity to obtain experience with a wide variety of clinical presentations, as patients are referred to MCC from nearly every CHOC medical specialty, including Neurology, Endocrinology, Gastroenterology, Oncology, Pulmonology, and many others. One of the main goals of MCC is to reduce barriers to accessing mental health services for CHOC patients and services are provided to patients with all insurance types, in-person or via telehealth, and using interpreters or bilingual clinicians as needed. Interns will provide psychodiagnostic evaluations to patients referred to MCC, score and interpret standardized intake questionnaires, evaluate and provide same-day feedback to patient/family whether a) they are a good fit for MCC short-term therapy model (4-16 sessions), b) a referral to community clinic for longer-term services is most appropriate, c) patient does not currently require therapy services (CHOC Psychology can be on ‘stand by’ in case future needs arise), or d) some combination of a, b, and c, and provide short-term therapy (4-16 sessions) to patients deemed appropriate for MCC services. Patients are seen in MCC when there is a mental health condition related to medical diagnosis. Examples include: Adjusting to a new medical diagnosis, Increased depression, anxiety, etc. that are negatively impacting medical adherence, Overall medical adherence concerns, Trauma related to medical procedures, hospitalizations, etc., and Impact of living with a chronic medical condition on functioning (e.g. social/peer relationships, school reintegration, young adulthood milestones). Interns will also administer, score, and interpret standardized questionnaires approximately 2 sessions prior to discharge to guide discharge planning and to track clinical outcomes. Interns on this rotation will have the opportunity to coordinate care with multidisciplinary teams of pediatricians, nurse practitioners, medical residents, social workers, case managers and resource specialists. (Supervisors: Anton Petrenko, Ph.D., Anita Saavedra, Psy.D., Amanda Suplee, Ph.D.)
*Interns Choose either the Emergency Department or Consultation-Liaison Rotation
Emergency Department Rotation (6-month rotation): Interns on the Emergency Department rotation will work in the Emergency Department (ED) with patients who are presenting with social, emotional, and/or behavioral issues. Interns will learn about the most common behavioral health concerns (e.g., suicidal ideation, aggressive behaviors) that present to the emergency department. In the ED, interns will participate in diagnostic evaluations of children presenting in a psychiatric crisis and help to determine what level of care is needed (such as admission to an inpatient psychiatric unit or intensive outpatient services) and what are appropriate discharge recommendations. Interns will administer, score, and interpret standardized assessment measures to inform disposition planning. In the ED, interns will also participate in an evidence supported family-based intervention for children in crisis. Interns will work with a variety of health care providers, including physicians, residents, nurses, and case managers. There will be a particular focus on the use of Motivational Interviewing (MI) elements. (Supervisors: Vicky Bouche, Ph.D.,Meredith Dennis, Ph.D.)
Consultation-Liaison (CL) Service Rotation (6-month rotation): Interns will obtain a breadth of experience with a variety of medical diagnoses comes from an intensive 6-month rotation with the consultation and liaison service at CHOC. Interns not only serve as consultants for the patient and/or family, but for the medical team, around a variety of issues. Consults are requested by attending physicians, residents, nurses, or other health care providers for children who are hospitalized for medical diagnoses and are experiencing concomitant psychological problems. Referral questions range from behavioral emergencies to suicide attempts requiring safety assessment to coping with an initial diagnosis to concerns for possible somatization disorders to adherence to complicated medical regimens to parental discipline to coping with death and dying issues. Medical diagnoses also run the gamut from diabetes to epilepsy to pain disorders to gastrointestinal disorders to autoimmune disorders to oncology to somatic presentations with unknown etiology. Interns will conduct initial diagnostic evaluations. After an initial assessment, interventions may range from a referral for outpatient psychotherapy to referrals for psychological or neuropsychological assessment to interventions with the child and/or family while in the hospital to consultation and interventions with the medical team. Interns participate on a general consultation service one and a half days a week with a faculty supervisor. Interns will learn to conduct a brief clinical evaluation, formulate an impression, and formulate disposition plans. While cases can be complex, interns always work with a supervising faculty member, are part of a consultation liaison team which includes psychology attendings, psychology postdoctoral fellows, and another psychology intern, and participate in weekly CL rounds. The CL team also includes child and adolescent psychiatry fellows and psychiatry attendings. It is a busy consultation service, so you will be able to see 2 or more cases per week on average while on the service. (Supervisors: Maleia Mathis, Ph.D., Kristen Yule, Ph.D.)
Psychological Assessment Rotation (6-month rotation): All interns will participate in 6 months of assessment experience during the internship. During the assessment core rotation, interns will complete a minimum of 4-6 assessments. Interns will complete psychological diagnostic evaluations within our Thompson Autism and Neurodevelopmental Center (TANC) or within our Early Childhood/Neurodevelopmental Evaluation Clinic.
At TANC, interns will conduct evaluations for children 6 years and younger with suspected neurodevelopmental disorders. The TANC Assessment Clinic receives a wide variety of referrals regarding suspected neurodevelopment disorders, including autism, language disorder, ADHD, global developmental delay, and intellectual disability. Interns will participate in multidisciplinary assessment clinic, working with neurologists, developmental/behavioral pediatricians, speech therapists, and occupational therapists to assess and provide recommendations for children with NDD. Interns will have proficiency with a variety of assessment instruments, referral questions, ability to provide feedback to children and families, and the ability to recognize when to seek consultation. (Supervisors: Lauren Couch, Ph.D., Esther Hong, Ph.D., Myranda Flordelis, Psy.D.)
Interns working within the Early Childhood/Neurodevelopmental Evaluation Clinic will complete psychological diagnostic evaluations and play-based assessments within our Early Childhood Clinic (ages 0-8 years) and neurodevelopmental evaluations for young children within our Neurodevelopmental Assessment Clinic either as part of a neurodevelopmental clinic or as part of their routine medical care. During the assessment core rotation, interns will complete 3 early childhood assessments per month and 1-2 neurodevelopmental evaluations per month. Interns will also have the opportunity to follow 1 case at a time for implementation of interventions based upon the diagnostic evaluation within the Early Childhood Clinic. The Early Childhood and Neurodevelopmental Assessment Clinic receive a wide variety of referrals, including concerns for developmental delays, language disorders, ADHD, Autism, and other neurodevelopmental concerns, motor difficulties, sleep difficulties, feeding difficulties, concerns with elimination disorders, parent-child interactions, parent management strategies, and challenging behaviors. The general approach adopted in the clinic is one of hypothesis testing and testing to the referral questions (e.g., baseline evaluation, routine monitoring due to the medical condition, specific referral question from the family/medical team). Interns will gain proficiency with a variety of assessment instruments, referral questions, ability to provide tailored feedback to children and families, and the ability to recognize when to seek consultation. In some cases, you will also work with the child’s rehabilitation therapists, community agencies, and/or school in order to assist them in appropriate educational planning and may attend IEP meetings. (Supervisors: Marni Nagel, Ph.D., Amanda Suplee, Ph.D.)
Behavioral Emergency Services/On Call: A distinctive feature of our program is that all interns receive training in managing behavioral emergencies through the provision of consultation services to the CHOC Emergency Department and hospital inpatient medical units. Interns may also have the opportunity to take call 1-3 days throughout the training year for high-risk consults. Trainees are always paired with a faculty member for this coverage. High risk consults include assessment of suicide risk or acute mental status changes. Interns will conduct a brief clinical interview, provide crisis intervention and immediate disposition plans for patients with suicidal ideation, potentially aggressive behaviors, and possible psychosis. This training experience helps to increase your competence and comfort in assessing and managing behavioral emergencies.
Specialty Rotations
Specialty rotations are designed to be an in-depth experience within a specific area. By focusing on a single medical service for six months, interns have the opportunity to become an integral part of the medical team. Interns will play a central and vital role in providing assessment and psychosocial interventions and consulting with the medical team. Rotations may vary each year, but at least 4 of the following rotations will be offered each year. Interns complete two 6-month specialty rotations during the internship year.
Possible rotations may include:
- Eating Disorders
- Emergency Department
- Endocrinology
- Integrated Primary Care
- Pulmonology
Interns on the Eating Disorders rotation spend one day per week within a pediatric inpatient medical setting at CHOC at Mission Hospital. Interns deliver services to children and adolescents admitted for medical stabilization for their eating disorder. The rotation includes conducting comprehensive initial intakes, as well as follow-up interventions for a variety of eating disorders including Anorexia Nervosa, ARFID, and Bulimia Nervosa. Furthermore, interns have the opportunity to develop skills in utilizing an Family-Based Treatment (FBT) approach within an inpatient setting (an evidence-based treatment for eating disorders). Interns provide parent and patient psychoeducation, individual therapy with parents and patients, and facilitation of group meals and group therapy. Interns are integrated into the Eating Disorders multidisciplinary team, which includes physicians, nurse practitioners, dieticians, social workers, case managers, and child life specialists (Supervisor: Katelyn Anderson, Ph.D, Melanie Delanoy, Ph.D., Hannah Steinberg, Psy.D.).
Emergency Department Rotation: Interns who choose to do the Consultation-Liaison rotation as a core rotation can choose to do the Emergency Department rotation as a specialty rotation. Interns on the Emergency Department rotation will work in the Emergency Department (ED) with patients who are presenting with social, emotional, and/or behavioral issues. Interns will learn about the most common behavioral health concerns (e.g., suicidal ideation, aggressive behaviors) that present to the emergency department. In the ED, interns will participate in diagnostic evaluations of children presenting in a psychiatric crisis and help to determine what level of care is needed (such as admission to an inpatient psychiatric unit or intensive outpatient services) and what are appropriate discharge recommendations. Interns will administer, score, and interpret standardized assessment measures to inform disposition planning. In the ED, interns will also participate in an evidence supported family-based intervention for children in crisis. Interns will work with a variety of health care providers, including physicians, residents, nurses, and case managers. There will be a particular focus on the use of Motivational Interviewing (MI) elements. (Supervisors: Vicky Bouche, Ph.D.,Meredith Dennis, Ph.D.)
Interns on the Endocrinology rotation will participate in the Endocrine Clinic (Type-I and Type-II Diabetes clinics), with a variety of health care providers including physicians, nurses, case managers, nutritionists, social workers, and diabetes nurse educators. Interns will play an integrated role in a multidisciplinary diabetes clinic by conducting depression screenings and providing same-day consultation upon referral. Interns will engage in conducting brief psychological screening for the purpose of identification of any mental health problems that may need further psychological assessment, ensure appropriate risk/safety assessment, and provide appropriate recommendations and referrals. Interns are expected to provide the endocrinologists with verbal feedback after screening a patient as well as complete a brief electronic report. Interns will also contribute their professional opinion and expertise in monthly psychosocial rounds and maintain involvement in ongoing program development initiatives (curriculum development for therapy and/or group protocols, community engagement and education, etc.). Interns also will have the opportunity to provide short-term outpatient treatment geared towards adherence interventions for patient’s screened/referred to psychology (Supervisor: Mercedes Palacios, Ph.D.).
The Integrated Primary Care rotation aims to reduce barriers in accessing mental health services for a diverse and underserved population through integration into CHOC’s pediatric clinics throughout Orange County. This rotation offers the unique opportunity to be families’ first introduction to psychological services and will provide skill development in a fast-paced multidisciplinary environment through various clinical experiences. Interns will provide targeted mental health evaluations utilizing a “warm handoff” which may result in psychoeducation, skill building, and referrals to community mental health resources; provide brief outpatient follow-ups in clinic (30 minutes or less); co-lead psychoeducational groups targeted towards parents and patients in our primary care clinics; and work closely with the medical team to provide education, recommendations, and care coordination. Interns will acquire skills with regard to the evaluation of risk and safety concerns and safety planning within a primary care setting. Interns also will gain experience working with culturally and linguistically diverse patients across the developmental spectrum and develop a greater understanding about barriers to accessing care. Interns on this rotation will have the opportunity to work within a multi-disciplinary setting with a team of pediatricians, nurse practitioners, medical residents, social workers, case managers and resource specialists (Supervisor: Sarah Ruiz, Ph.D.).
Interns on the Pulmonology rotation work closely with the multidisciplinary Pulmonary sleep team, with a focus on patients with sleep disorders. Interns will participate in the Sleep Apnea Team clinic with a variety of health care providers, including physicians, nurses, case managers, social workers, respiratory therapists, and polysomnography sleep technicians. As the psychological consultant in these clinics, you learn to triage, assess patients, provide brief interventions, and conduct disposition planning with a fast-paced clinic setting. Interns receive training in cross-cutting issues in pediatric psychology, including adherence, pain, procedural anxiety/distress, family functioning, adjustment to illness, and depression/anxiety superimposed on chronic illness. Within the sleep apnea clinic, interns will conduct initial and follow up evaluations for children and adolescents with mild-to-severe obstructive sleep apnea (OSA) and assist children and families in improving adherence to and tolerance for prescribed PAP (positive airway pressure) treatment. Interns refine behavioral modification and desensitization skills to promote Positive Airway Pressure (PAP) adherence for patients who are having difficulty tolerating prescribed treatments. Additionally, patients often have multifactorial sleep disorders, and the intern works as part of the team to evaluate sleep disorders and determine treatment recommendations. Interns implement motivational interviewing techniques to assist with providing psychoeducation, assessing readiness for change, and problem-solving around potential barriers to adherence and other change behaviors. Pending scheduling availability, there may be an opportunity to participate in the general sleep psychology and sleep insomnia clinic as well, where interns will further develop acumen of comprehensive sleep evaluations and offering behavioral interventions to promote optimal sleep, including sleep hygiene and stimulus recommendations (Supervisor: Marc Chaney, Psy.D.).
Additional Clinical Activities
Optional Training Experiences:
Our doctoral internship training philosophy is to meet interns’ professional development needs to the extent possible. We can offer brief exposures to additional patient populations, clinics, or mental health service lines. Interns are encouraged to ask about different possibilities to tailor their training, and every effort will be made to accommodate them, as long as the proposed modification to the training plan permits the acquisition of all the core competencies of the internship program. Generally, these opportunities will be available as a brief 1-2 time exposure within a ½ day timeframe.
At the time of this writing, there are additional pediatric experiences available in gastrointestinal disorders, hematology, young child, gender identity clinic, and intensive outpatient programming. Interns have the opportunity to work with children and adolescents on issues centering around compliance with medical regimens, coping with the demands of the disease, pain management, and other psychosocial issues involved with chronic illness.
All medical areas have highly diverse patient populations. In addition, trainees will have the opportunity to develop skills working with interpreters to improve the care provided to patients in the hospital. Interns are trained in pertinent culture-specific practices. This training includes a seminar in Diversity issues.
Training Opportunities for Spanish Speaking Interns:
Our doctoral internship in health service psychology is dedicated to providing training opportunities for interns who speak Spanish. These experiences include the ability to conduct assessments in Spanish utilizing our library of assessment instruments that have been developed and normed with Spanish speaking populations.
In addition, interns who speak Spanish have the opportunity to participate in a bi-monthly seminar, CHiSPA, coordinated by Mercedes Palacios, Ph.D. and Anita Saavedra, Psy.D., with several bilingual faculty and staff members as guest presenters. This bi-weekly seminar for interns, fellows, and practicum students with Spanish language proficiency, focuses on increasing professional skills in and comfort with conducting psychological services, including assessments, consultations, and interventions in Spanish. Activities include working on psychological vocabulary, practice in discussing cases and case conceptualizations in Spanish, diversity factors that may impact evidence-based practice for Spanish speaking populations, and discussions of health psychology, health literacy, adherence, and perceptions of medical and mental health diagnoses and treatments with Spanish speaking patient populations. The goal of the seminar is to provide support and build on participants’ individual strengths.
We currently have 14 full time licensed psychologists who are bilingual in Spanish, in addition to bilingual and bicultural department mental health providers.
Supervision
All trainees receive a combination of individual and group supervision (a minimum of four hours) per week. Supervision occurs on an individual basis, during group rounds, within clinic settings, and within the Training Program seminars. All supervision is performed by departmental faculty members who meet the California Board of Psychology requirements and CHOC Hospital’s Medical Staff qualifications. Supervisors will conduct direct observations of your clinical work on all rotations at least once during each formal evaluation period either through live, direct supervision or video recording review.
Interns are offered at least two hours of individual supervision per week for ongoing outpatient therapy cases and specialty rotational experiences. Supervision of the consultation-liaison service is handled with both individual supervision and via group supervision (rounds). Rounds are led by licensed psychologists and at times co-led by a board-certified child & adolescent psychiatrist. The amount and frequency of this supervision will vary depending on the complexity and number of consults received. Typically, individual consultation-liaison supervision occurs for 1 hour per week plus additional time as needed, and group consultation-liaison supervision occurs for 1 hour per week. Additionally, consultation services are often provided using a co-assessment and co-treatment model, especially for high risk and complex consults. Therefore, interns are able to observe their supervisors providing psychological services. There also may be opportunities to participate in co-therapy with supervisors and receive immediate feedback based on direct observation of clinical skills. Assessment supervision is provided as the case progresses, and is at least 1 hour per week. Additionally, the supervisor is often present for intakes and feedbacks and will be present for testing as needed. Furthermore, interns on the emergency department rotation also receive 1 hour of individual or group supervision per week, in addition to daily case-based supervision. Supervision is also provided informally during medical rounds on major rotations. In addition, there is a strong postdoctoral fellow presence who can also provide case consultation and professional development under the supervision of a licensed supervisor. Supervision and responsibility for the patients will ultimately be the responsibility of a licensed clinical psychologist on staff.
You will be assigned one outpatient therapy Medical Coping Clinic supervisor who will work with you throughout the year. This supervisor will provide continuity throughout the year and will also serve as a professional mentor.
You will be assigned one assessment supervisor who will work with you throughout the 6-month assessment experience. Within the 6-month experience, you will complete a minimum of 4-6 assessments. Your supervisor will provide continuity on these cases and mentor you in the development of your assessment skills.
You will be assigned one emergency department supervisor who will work with you throughout the 6-month emergency department rotation, and two specialty rotation supervisors (6-months each) who will work with you throughout each of your 6-month specialty rotation experiences.
Supervision Experiences:
You will be provided with an opportunity to supervise practicum students. Training in the provision of supervision will be provided through didactic seminars and formal supervision of your own provision of supervision. Supervision and responsibility for the patients will ultimately be the responsibility of a licensed clinical psychologist on staff. You may be expected to video record supervision sessions with your supervisees to share with your supervisor in order to develop your own supervision competencies.
Training Program Seminars
Required
- Child Adolescent Assessment Seminar (CAAS: 2 hours twice monthly for 6 months)
- Child Adolescent Psychological Principles Seminar (CAPPS: 2 hours twice monthly for 6 months and 2 hours weekly for 6 months)
- Professional Practice Seminar (2 hours twice monthly)
Optional
- CHiSPA (bi-weekly)
- Advanced Neuropsychology Seminar (bi-weekly)
- Pediatrics Grand Rounds (weekly)
- Morning Report (daily)
Content of required seminars is focused on more practical applications of evidence based approaches, with a specific emphasis on medically complex children. A didactic element is included in all seminars. Professional issues are addressed throughout the training year. Outside speakers with a particular area of expertise are invited to present in several of the seminars. Trainees may also attend the CHOC Grand Rounds and/or other teaching rounds as time permits.
Child Adolescent Assessment Seminar (CAAS): This bi-weekly 2-hour seminar focuses on topics relevant to assessment and evaluation within the practice of Psychology with children and adolescents. Presentations will focus on various evidence-based assessment approaches for youth, as well as assessment considerations when working with specialized pediatric populations. We will also have guest speakers from other disciplines that psychologists frequently collaborate with on multidisciplinary teams (Coordinators: Marni Nagel, Ph.D.).
Child Adolescent Psychological Principles Seminar (CAPPS): This weekly to bi-weekly 2-hour seminar focuses on topics relevant to the practice of Psychology with children and adolescents. Presentations will focus on various evidence-based treatments for youth, as well as use of these treatments in specialized pediatric populations. We will also have guest speakers from other disciplines that psychologists frequently collaborate with on multidisciplinary teams. This will be an opportunity to learn how different disciplines function both at CHOC and as a broader specialization with youth and how psychologists can help integrate skills on a team to better serve the mental health needs of children and adolescents (Coordinator: Marni Nagel, Ph.D.).
Professional Practice Seminar: This seminar consists of three main topic areas; diversity, ethics, and supervision. It is designed to focus on learning and application to your clinical work that supports increased competency in these three areas. The diversity series within the seminar are interactive in nature and consists of self-exploration activities, exploration of the surrounding community (through research and an experiential activity), presentations from professionals as well as trainee case presentations. While we expect diversity awareness to permeate all of your work throughout the year, this seminar is designed to help you develop your model of learning and practice (Coordinator: Ana d’Abreu, Ph.D.). The ethics series within the seminar focus on cases in medical settings that bring a multitude of ethical challenges, which can be complex and difficult to identify a clear path forward. In this seminar, faculty present cases they have worked on that have presented ethical challenges. In these interactive presentations, faculty and interns discuss systems and strategies to assess ethical dilemmas and determine courses of action (Coordinator: Marni Nagel, Ph.D.). The supervision series within the seminar are focused on models and theories of supervision, roles of the supervisor and setting up supervisory relationships, assessing supervisee competency, and providing feedback, including evaluative feedback (Coordinator: Marni Nagel, Ph.D.).
Interns make formal case presentations in the Child Adolescent Psychological Principles Seminar (one therapy case) and Child Adolescent Assessment Seminar (one assessment case), as well as more information presentations/consultations in Professional Practice Seminar (diversity case presentation, ethics case presentation) and Advanced Neuropsychology Seminar (case consultation) and CHiSPA (case consultation).
Research Opportunities
The training faculty strongly believes that the primary focus of internship training is on clinical work. We also believe that science underlies our practice of psychology. The Department of Pediatric Psychology at CHOC does have a number of ongoing clinical research studies which interns are exposed to and may be able to take part in limited ways. Postdoctoral fellows are more integrally involved in these research projects.
The UCI Center on Stress and Health is part of the Department of Anesthesiology and Perioperative Care, at the University of California-Irvine (UCI) and Department of Pediatric Psychology at CHOC (CHOC). The Center on Stress and Health is a collaborative group from diverse areas in medicine, nursing, and psychology. Under the Direction of Dr. Zeev Kain, and Dr. Michelle Fortier, the center conducts cutting edge research on children’s health with particular interests in medical anxiety and pain. The Center on Stress and Health was first established by Dr. Kain under the name, the Center for the Advancement of Perioperative Health (CAPH) which relocated from Yale University to UCI/CHOC in July 2008. The multi-disciplinary research team has a number of ongoing federally funded projects examining perioperative pain and anxiety as well as procedural pain and anxiety.
As only a couple of examples of clinical research in the Department, the oncology team has developed a psychosocial screener measure to examine longitudinal psychosocial effects of having cancer. The neuropsychology program is looking at long term outcomes in children who receive epilepsy surgery, long term outcomes of children with cardiac conditions, and the cognitive effects of treatment for childhood cancer with a particular emphasis on differing effects for bilingual children. The feeding program is looking at quality of life outcomes for children who undergo an intensive intervention to move from g-tube feedings to oral feeding. The sleep program is looking at improving adherence for PAP treatment among children and adolescents who have difficulty tolerating PAP. The CF program is looking at screenings for depression and anxiety, and linking to resources among patients diagnosed with CF and their parents.
Training Model
Our doctoral internship in health service psychology training model is that of scholar-practitioner. Consistent with this model, the focus of the training program is on the provision of direct patient care utilizing the most up-to-date knowledge, skills and interventions coupled with the evaluation of the efficacy of those interventions and continued planning to improve those services. The mission of our training program is to provide high quality pediatric psychology training to advanced students in preparation for independent practice. In order to achieve our mission, we assist in the development of a range of assessment and therapeutic skills as well as the development of a unique professional identity that builds on the individual skills and abilities that each intern brings to the program at entry. The internship program philosophy of training is that intensive experiential activities with patients are crucial to the development of a unique therapeutic style and therapeutic skill set. The development of this individual style can be a cornerstone in the ultimate development of your own unique individual professional identity. Through these intensive experiences interns can take the skills learned in their graduate programs and further refine them and continue to develop their own unique and individual style of professional practice.
The majority of current staff members were trained in the scientist-practitioner model and see the inclusion of empirical work as a necessary component for the competent treatment of psychological problems. We strive to provide interns with a breadth and depth of training experiences in the context of utilizing innovative scientific information to guide their treatment planning, conceptualization, and delivery. All staff members remain actively involved in scientific associations, continuing education, and reviewing the relevant literature, in order to constantly improve the quality of their work and supervision. Many staff also are involved in ongoing clinical research studies.
Training Purpose and Objectives
The purpose of our doctoral internship in health service psychology is to provide a training experience to advanced graduate psychology students within a multi-disciplinary setting that meets the qualifications of field experience in Ph.D./Psy.D. programs and licensing requirements for the Board of Psychology of the State of California (as well as those of other states).
The primary purpose of the internship at CHOC is to prepare psychology graduate students for the professional practice of pediatric and child psychology in a variety of settings (e.g. hospital, school, clinic, and private practice), with a special emphasis on practice in medical settings. Following the field of Pediatric Psychology, the internship focuses on addressing the relationship between children’s physical, cognitive, social, and emotional functioning and their physical well being, including maintenance of health, promotion of positive health behaviors, and treatment of chronic or serious medical conditions. We view the training year as a time for intensive clinical experience. Although we do not see interns as having the time to complete additional research projects (as well as their own dissertation) during their own internship year, we do require ongoing scholarly activity, such as literature review, critical thinking, and appropriate application of the pediatric psychology literature.
Through our program, interns will learn to assess the psychosocial impact of acute and chronic illness in children and their families. Interns will become proficient in psychodiagnostic evaluation. They also will be exposed to neurodevelopmental/ neuropsychological testing within a medical population and know how to determine the need for further cognitive assessment. Interns will gain significant experience in hospital consultation and liaison skills, which includes providing inpatient interventions and giving feedback to physicians and other medical professionals.
Our program is designed to provide more structure at the beginning of the year, and for interns to play an increasingly independent role towards the end of the year. During this year of critical transition from a graduate student to a professional psychologist, we encourage trainees to develop a professional identity, professional values, and a professional demeanor.
We fully anticipate that interns graduating from our program will be prepared for entry-level independent practice in child and adolescent psychology depending upon individual state licensure requirements and/or to begin specialty training at the postdoctoral fellow level depending upon individual career objectives. Many of our graduates go on to complete formal postdoctoral fellowships in order to further specialize in a particular area, others go on to assistant professorship positions, and others become private practitioners.
Total Program Hours and Licensure
Licensure in the state of California requires 1500 Predoctoral and 1500 Postdoctoral hours of Supervised Practice, as well as successful completion of the national written exam (EPPP) and a written exam in California Professional Law and Ethics (CPLEE). Satisfactory completion of the doctoral internship at CHOC exceeds this requirement and provides 2000 hours of Doctoral Supervised practice. CHOC interns can anticipate that their weekly responsibilities will be approximately 40 – 45 hours per week. This time estimate includes clinical service, supervision, seminars, administration, scoring, documentation, and report writing.
APA Accreditation
Our internship program is APA accredited. We completed our virtual site visit in May 2021, and completed our on-site accreditation verification visit in December 2022. Our program received accreditation for ten years during our last accreditation cycle, with our next site visit in 2031.
The American Psychological Association Office of Program Consultation and Accreditation can be reached at:
750 First Street, NE
Washington, DC 20002-4242.
Telephone: (202) 336-5979
TDD/TTY: (202) 336-6123
www.apa.org
Evaluations
Informal evaluations are conducted throughout the year; formal evaluations are conducted after the first quarter of the year (3 months), again at mid-training year (6 months), and at the end of the training year (12 months). Formal evaluations will include a form of direct supervision, either live or via video recording review. Informal evaluations may include direct supervision as well. These evaluations are conducted by training teams which consist of the interns’ supervisors across the different domains of training. These evaluations look at the trainees’ strengths in a variety of areas including diagnostic skills, interventions, assessment, professional practice, awareness of multicultural practice and response to supervision. Evaluation results are shared with the trainees so that goals can be defined and planned for and refinements in trainee performance can occur. Trainees are also asked to evaluate their supervisors and the Training Program annually. Supervisor and Training Program evaluations are used to review and clarify rotation strengths and weaknesses, supervisor performance, and program efficacy.
Educational Services
Both interns and fellows can use Burlew Medical Library, located on the St. Joseph Hospital campus. A selection of professional books, journals, and audiovisual materials are available. Literature searches are free. Professional databases include Ovid, the National Library of Medicine MEDLINE, HEALTH and CINAHL. Access can be accomplished remotely. The Department of Pediatric Psychology has an assortment of professional books and journals germane to professional work at CHOC. Copying and multi-media services are available for presentations.
Internship Location
CHOC is located in central Orange County, placing it less than an hour drive from the City of Los Angeles and about 30 minutes from the Pacific Ocean. Mountain resorts and the California desert are less than two hours away. The Southern California climate is very moderate all year round. Housing costs in Orange County tend to be on the high average side, but are often more affordable than in other major metropolitan areas. Orange County offers great diversity in terms of its population, with significant Latinx, Vietnamese, Indian, and Filipino populations.
Salary and Benefits
- Interns: $52,956/year, overtime is paid for time over 40 hours a week.
- Medical, Dental and Vision Insurance (after first full month of employment)
- Paid time off (total of 21 days for educational/vacation/sick leave (15 days) and departmental closures/holidays (7 days)).
- Paid sick leave (total of 5 days per fiscal year, accrued at 1 hour per 30 hours worked)
- 3 educational days (for activities such as attending or presenting at conferences, defending your dissertation) in addition to paid time off listed above.
- Each intern has individual computers with internet access. Toys and games are also available for work with children.
- Video cameras and digital audio recording devices are available on site to facilitate supervision of more challenging cases. Live video streaming is also available for live supervision.
- Interns receive free parking.
Application Procedure
The application deadline for interns is November 1, 2025 in order to begin training on August 24, 2026. Our department participates in the computerized matching program for internship applicants. Information is available through APPIC (www.appic.org). Applications can be downloaded from the APPIC web site.
Please include the following in your application:
- Completed AAPI online application (which can be obtained from https://aapicas.liaisoncas.com/applicant-ux/#/login)
- Curriculum vitae;
- Three letters of recommendations from graduate faculty and/or clinical supervisors (at least one letter should be from a supervisor who has direct knowledge of your clinical work and at least one letter should be from a core member of your graduate faculty), these should be submitted with your AAPI online application process;
- Completed neuropsychological or psychological test report on a child or adolescent (with identifying information removed). This is uploaded as supplemental material with your electronic AAPI.
Please address application inquiries to:
Marni Nagel, Ph.D., Director Psychology Training Program, Senior Psychologist
Department of Pediatric Psychology
CHOC Children’s Hospital
1201 West La Veta Ave
Orange, CA 92868-3874
Phone: (714) 509-8481
Fax: (714) 509-8756
Email: [email protected]
Virtual interviews will be held in January and are by invitation only in order to minimize the significant financial and time burden for applicants. You will be informed whether you will be invited for an interview by December 15, 2025 (every effort will be made to inform applicants earlier). The interview process includes a semi-structured interview. This format allows everyone the same opportunity to show all of the skills and knowledge you have gained over the course of your graduate training. It also ensures that we ask you about all important areas. Time is also scheduled for more open-ended discussions where you can ask questions about our internship site. We also schedule time for you to talk to with our current trainees. For those applicants who indicate you speak Spanish, a portion of the interview will be conducted in Spanish. With your permission, we would like to take a picture at the interview in order to assist the memory of the selection committee. This is a totally voluntary process, and all applicants are welcome to opt out of the photograph.
As an institution CHOC applies to all provisions of equal opportunity/affirmative action employment practices. The internship is open to all qualified individuals regardless of irrelevant factors such as culture, race, ethnicity, disability, gender, sexual/gender orientation or religion. Applicants from minority and diverse cultural backgrounds are encouraged to apply.
Application Requirements
Admission requirements for interns include advanced candidacy, good standing in their graduate program, and current enrollment in an APA accredited clinical, counseling, or school psychology program; two years of part-time clinical placements, one year of which must include services to children; a background in basic psychological testing measures (e.g. IQ, achievement, objective and projective personality measures); and finally, exposure to and interest in pediatric psychology which can be demonstrated through coursework, clinical placement, or research. Discussion of your interest in pediatric psychology training can be included in your essays and/or cover letter.
The CHOC doctoral internship training program in health services psychology abides by the APPIC policy that no person at this training facility will solicit, accept, or use any ranking-related information from any intern applicant.
Applicants matched to the internship should understand that prior to beginning the internship they will be required to successfully pass a required brief medical examination, which includes a drug test. TB testing will also be required. Applicants will also undergo a required background test which CHOC requires of all employees in order to ensure the safety of our pediatric patients.
Questions
Programmatic Questions: Please email or call with any questions about the program. Please direct any questions about programmatic issues to Dr. Marni Nagel at [email protected]. Additionally, you may call (714) 509-3455.
Questions about application status: If you have questions regarding the status of your application (e.g. is it complete or what is missing), please email Gabriella Romero at [email protected] or call 714-509-3455 and ask for Gabriella.
Pediatric Psychology Department Faculty and Staff
Heather Huszti, Ph.D., Chief Psychologist, Licensed Psychologist
- Clinical Psychology, Texas Tech University
- Clinical/Training Interests: Hematology, Adherence, Consultation and Liaison services, Pediatric critical care
Julie Moghal, Ph.D., Director, Department of Psychology, Licensed Psychologist
- Clinical Psychology, University of Toledo
- Clinical/Training Interests: Law and ethics, Mentoring and supervision, Autism, Young child/feeding
Marni Switkin Nagel, Ph.D., Director Psychology Training Program, Senior Psychologist, Licensed Psychologist
- Clinical and Developmental Psychology, University of Maryland Baltimore County
- Clinical/Training Interests: Assessment and intervention with infants and young children, Neurodevelopmental assessment, Sleep medicine, Neonatal critical care, Chronic illness, Pain management
Baleska Alfaro, LMFT, Licensed Marriage and Family Therapist, Project HEALTH
Barbara Allen, LMFT, Licensed Marriage and Family Therapist, Intensive Outpatient Programming
Darcy Alcantara, Ph.D., Licensed Psychologist
- Clinical Psychology, University of Massachusetts- Boston
- Clinical/Training Interests: Integrated Primary Care, Diversity Training, Working with Latinx Populations
Adrianne Alpern, Ph.D., Licensed Psychologist
- Clinical Psychology, University of Miami
- Clinical/Training Interests: Cystic Fibrosis, Adherence, Diabetes, Gender identity and diversity, Adjustment and coping with chronic illness
Katelyn Anderson, Ph.D., Licensed Psychologist
- Counseling Psychology, University of Oregon
- Clinical/Training Interests: Eating Disorders, Consultation-Liaison, Gender identity and diversity
Sandra Avila, Psy.D., Licensed Psychologist
- Clinical Psychology, CSPP Alliant International University, Alhambra
- Clinical/Training Interests: Pediatric Psychology, Integrated Primary Care, Mental Health prevention and early intervention
Vicky Bouche, Ph.D., Licensed Psychologist
- Clinical Psychology, Palo Alto University
- Clinical/Training Interests: Acute Care, Crisis assessment and intervention, Consultation-Liaison
Esmeralda Cardenas, LCSW, Licensed Social Worker, Project HEALTH
Ava Casados, Ph.D., Licensed Psychologist
- Clinical Psychology, Yale University
- Clinical Training Interests: Community education, Integrated Primary Care, Law and Ethics, Health disparities
Marc Chaney, Psy.D., Licensed Psychologist
- Clinical Psychology, Adler University
- Clinical/Training Interests: Pediatric Psychology, Behavioral Sleep Medicine, Adherence
Elisa Corrales, Ph.D., Licensed Psychologist
- Clinical Psychology, University of Rochester
- Clinical/Training Interests: Childhood trauma, PCIT, children’s chronic illness
Lauren Couch, Ph.D., Licensed Neurodevelopmental Psychologist
- School Psychology, University of California, Riverside
- Clinical/Training Interests: Autistic Spectrum Disorders
Ana d’Abreu, Ph.D., Licensed Psychologist
- School Psychology, Texas A&M University
- Clinical/Training Interests: Social-emotional prevention programs, School-based mental health services, Resilience & acculturation factors in youth, Diversity, Equity, and Inclusion
Melanie Delanoy, Ph.D., Licensed Psychologist
- Clinical Psychology, University of Arizona
- Clinical/Training Interests: Eating Disorders, Supervision
Meredith Dennis, Ph.D., Licensed Psychologist
- Clinical Psychology, Loma Linda University
- Clinical Training Interests: Acute psychiatric disorders, Emergency Department, Crisis Intervention and Management, Autism Spectrum Disorders
Myranda Flordelis, Psy.D., Licensed Neurodevelopmental Psychologist
- Clinical Psychology, California School of Professional Psychology at Alliant International University Los Angeles
- Clinical/Training Interests: Autistic Spectrum Disorders
Ana-Mercedes Flores, Ph.D., Licensed Pediatric Neuropsychologist
- Clinical Psychology, Eastern Michigan University
- Clinical/Training Interests: Neuropsychology, Neurodevelopmental evaluation
Wendy Gray, Ph.D.,ABPP, Licensed Psychologist
- Clinical Psychology, University of Florida
- Clinical/Training Interests: IBD, Pediatric GI, Abdominal pain, Adolescent/Young Adult transition to Adult Care
Heather Hennrick, Ph.D., Licensed Pediatric Neuropsychologist
- Clinical Psychology, Eastern Michigan University
- Clinical/Training Interests: Epilepsy, Seizure Disorders, Pediatric neuropsychology
Gaby Hernandez, LCSW, Licensed Social Worker, MHIC
Esther Hong, Ph.D., Licensed Neurodevelopmental Psychologist
- Clinical Psychology, Louisiana State University
- Clinical/Training Interests: Autistic Spectrum Disorders
Jina Jang, Ph.D., Licensed Neurodevelopmental Psychologist
- Clinical Psychology, Louisiana State University
- Clinical/Training Interests: Autistic Spectrum Disorders
Annemarie Kelleghan, Ph.D., Licensed Psychologist
- Clinical Psychology, University of Southern California
- Clinical/Training Interests: Pediatric Psychology, Integrated Primary Care, Mental Health prevention and early intervention
Cindy S. Kim, Ph.D., ABPP, Licensed Psychologist
- Clinical Psychology, Biola University/Rosemead School of Psychology
- Clinical/Training Interests: Pediatric feeding disorders in infancy and early childhood, Young child mental health, Cochlear implants, and Developmental Disabilities
Carlos Konishi, Ph.D., Licensed Psychologist
- Clinical Psychology, University of Southern Mississippi
- Clinical/Training Interests: Coping and adjustment to chronic illness, Pediatric oncology, Diversity training
Mariam Ibrahim, Ph.D., Licensed Psychologist
- Clinical Psychology, Arizona State University
- Clinical/Training Interests: Integrated Primary Care, Diversity training
Michelle Lopez, LMFT, Licensed Marriage and Family Therapist, Project HEALTH
Karina Martinez, LMFT, Licensed Marriage and Family Therapist, Project HEALTH
Maleia Mathis, Ph.D., Licensed Psychologist
- Clinical Psychology, Loma Linda University
- Clinical/Training Interests: Consultation-Liaison, School based mental health, Diversity, Equity, and Inclusion
Chris Min, Ph.D., Licensed Psychologist
- Clinical Psychology, University of Maryland Baltimore County
- Clinical/Training Interests: Integrated Primary Care, Consultation-Liaison, Neurology, Sleep medicine
Sheila Modir, Ph.D., Licensed Psychologist
- Combined, Clinical-Counseling-School Psychology, University of California, Santa Barbara
- Clinical/Training Interests: Coping mechanisms and understanding resilience in the context of trauma for vulnerable populations
Kathryn Moffa, Ph.D., Licensed Psychologist
- Combined Clinical, Counseling, and School Psychology, University of California, Santa Barbara
- Clinical/Training Interests: School-Based Mental Health Services, Child Clinical Psychology, Pediatric Psychology
Shirin Mostofi, Ph.D., Licensed Psychologist
- Clinical Psychology, Loma Linda University
- Clinical/Training Interests: Intensive outpatient programming, Crisis Management, Acute Psychiatric Crises, Dialectical Behavior Therapy, Working with young children
Elizabeth Mu, LMFT, Licensed Marriage and Family Therapist, Intensive Outpatient Programming
Anton Petrenko, Ph.D., Licensed Psychologist
- Clinical Psychology, Northern Illinois University
- Clinical/Training Interests: Hematology, Pediatric Psychology, Coping with Chronic Medical Conditions, Adherence
Mercedes Palacios, Ph.D., Licensed Psychologist
- Clinical Psychology, Palo Alto University
- Clinical/Training Interests: Pediatric Psychology, Diabetes, Diversity Training, Working with Latinx Populations
Eric Proffitt, Psy.D., Licensed Psychologist
- Clinical Psychology, Azusa Pacific University
- Clinical/Training Interests: Hematology/Oncology/BMT, Consultation-Liaison, Eating disorders
Nancy Ramirez, LCSW, Licensed Social Worker, MHES
Jonathan Romain, Ph.D.,ABPP-CN, Licensed Pediatric Neuropsychologist
- Clinical Psychology, California School of Professional Psychology, Fresno
- Clinical/Training Interests: Epilepsy, Seizure Disorders, Pediatric neuropsychology, TBI and Concussion
C. Julieta Aguilera Rice, Ph.D., Licensed Psychologist
- Clinical-School Psychology, McGill University
- Clinical/Training Interests: Pediatric Psychology, Oncology, Diversity, Equity, and Inclusion
Kevin Rowen, Psy.D., Licensed Psychologist
- Clinical Psychology, CSPP at Alliant International University, Los Angeles
- Clinical/Training Interests: Acute Care, Crisis assessment and intervention, Intensive Outpatient programming, Dialectical Behavior Therapy
Sarah Ruiz, Ph.D., Licensed Psychologist
- Child Clinical Psychology, University of Minnesota, Institute of Child Development
- Clinical/Training Interests: Integrated Primary Care, Diversity training, Diversity, Equity, and Inclusion
Scott Ryan, LMFT, Licensed Marriage and Family Therapist, Intensive Outpatient Programming
Anita Saavedra, Psy.D., Licensed Psychologist
- Clinical Psychology, Pepperdine University
- Clinical/Training Interests: Pediatric Psychology, School-Based Services, Diversity Training, Working with Latinx Populations
Hannah Steinberg, Psy.D., Licensed Psychologist
- Clinical Psychology, PGSP-Stanford PsyD Consortium
- Clinical/Training Interests: Eating Disorders, Consultation-Liaison, Suicide assessment
Amanda Suplee, Ph.D., Licensed Psychologist
- Clinical Psychology, Loma Linda University
- Clinical/Training Interests: Early Childhood assessment and treatment, play-based assessment, Consultation-Liaison
Alexander Tan, Ph.D., ABPP-CN, Licensed Pediatric Neuropsychologist
- Clinical Psychology, Children’s Health & University of Texas Southwestern Medical Center (UTSW), Dallas
- Clinical/Training Interests: Neuropsychology, Cardiac neurodevelopmental concerns
Mery Macaluso Taylor, Ph.D., Licensed Psychologist
- Clinical Child Psychology, University of Kansas
- Clinical/Training Interests: Consultation-Liaison services, Chronic Pain, Latinx populations, Diversity Training
Micaela Thordarson, Ph.D., Licensed Psychologist
- Clinical Psychology, Pacific Graduate School of Psychology at Palo Alto University
- Clinical/Training Interests: Intensive outpatient programming, Crisis Management, Acute Psychiatric Crises
Carolina Eberhard Veira, LCSW, Licensed Clinical Social Worker, Project Health
Nicole Vincent, Ph.D., Licensed Psychologist
- Clinical Psychology, University of Miami
- Clinical/Training Interests: Anxiety in children and adolescents, Pain management, Tic disorders, Therapy with school-age children and adolescents, Disorders of sex development, Psychosocial and cognitive issues in pediatric oncology
Elicia Wartman, Ph.D., Licensed Psychologist
- Clinical Psychology, Loyola University Chicago
- Clinical/Training Interests: Pediatric GI Disorders, Pain Management, Consultation-Liaison
Tyler Womack, Ph.D., Licensed Neurodevelopmental Psychologist
- School Psychology, University of California Riverside
- Clinical/Training Interests: Autistic Spectrum Disorders
Elissa Wu, Psy.D., Licensed Psychologist
- Clinical Psychology, Wheaton College
- Clinical/Training Interests: Therapy with children and adolescents with co-occurring mental health and medical conditions, Trauma-Focused Cognitive Behavior Therapy
Psychiatry Faculty:
Hoang “Wayne” Nguyen, MD, Chief of Child and Adolescent Psychiatry, Medical Director, Mental Health Inpatient Center, Board Certified Child/Adolescent Psychiatrist
- Medical School, Texas A & M Health Science Center, Internship and Residency, University of Utah Medical Center
- Clinical/Training Interests: Child and adolescent psychiatry,
Psychosomatic Disorders, Developmental Disorders, Pain Medicine
Michael Chu, MD, Board Certified Child and Adolescent Psychiatrist
- Medical School, University of Maryland, School of Medicine
- Psychiatry Residency: University of Maryland Sheppard Pratt
- Fellowship: University of California, San Diego/Rady Children’s Hospital Clinical/Training Interests: Child and adolescent psychiatry, consultation liaison and emergency department.
Michael Hwang, MD, Board Certified Child and Adolescent Psychiatrist, IOP, Pediatric Psychology Continuity Clinic
- Medical School, New York University, Internship: Tulane University, Fellowship: University of California, Irvine
Laura Lai, MD, Board Certified Child and Adolescent Psychiatry, ASPIRE IOP
- Internship and Fellowship: University of California, Irvine
Uma Rao, MD, Board Certified Child and Adolescent Psychiatry, Director of Behavioral Research
Lavanya Wusirika, MD, Child and Adolescent Psychiatry, MHIC
- Fellowship: University of California, Los Angeles
Esther Yang, MD, Board Certified Psychiatry, Child and Adolescent Psychiatrist
- Internship and Fellowship: University of California, Irvine Medical School