Hirschsprung’s Disease
What is Hirschsprung’s disease?
Hirschsprung’s disease occurs when some of the nerve cells that are normally present in the intestine do not form properly while a baby is developing during pregnancy.
As food is digested, muscles move food forward through the intestines in a movement called peristalsis. When we eat, nerve cells that are present in the wall of the intestines receive signals from the brain telling the intestinal muscles to move food forward. In children with Hirschsprung’s disease, a lack of nerve cells in part of the intestine interrupts the signal from the brain and prevents peristalsis in that segment of the intestine. Because stool cannot move forward normally, the intestine can become partially or completely obstructed (blocked), and begins to expand to a larger than normal size.
What causes Hirschsprung’s disease?
Between the 4th and the 12th weeks of pregnancy, while the fetus is growing and developing, nerve cells form in the digestive tract, beginning in the mouth and finishing in the anus. For unknown reasons, the nerve cells do not grow past a certain point in the intestine in babies with Hirschsprung’s disease.
How often does Hirschsprung’s disease occur?
Hirschsprung’s disease occurs in 1 out of every 5,000 live births.
Who is at risk for Hirschsprung’s disease?
Hirschsprung’s disease occurs five times more frequently in males than in females, and children with Down syndrome have a higher risk of having the disease. There is possibly a genetic, or inherited, cause for Hirschsprung’s disease.
Why is Hirschsprung’s disease a concern?
Because a segment of the intestine lacks normal nerve cells, digested food and stool cannot move forward through that portion of the digestive tract. The intestine becomes blocked with stool, and the baby will be constipated, or unable to have normal bowel movements.
The obstruction (blockage) causes pressure on the inside of the intestine, causing part of the intestinal wall to wear thin. Eventually, a bacterial infection can develop in the digestive tract, causing serious problems.
What are the symptoms of Hirschsprung’s disease?
Most children with Hirschsprung’s disease show symptoms in the first few weeks of life. Children who only have a short segment of intestine that lacks normal nerve cells may not show symptoms for several months or years. The following are the most common symptoms of Hirschsprung’s disease. However, each person may experience symptoms differently. Symptoms may include:
- Not having a bowel movement in the first 48 hours of life
- Gradual bloating of the abdomen
- Vomiting green or brown fluid.
Children who do not have early symptoms may also present the following:
- Constipation that becomes worse with time
- Loss of appetite
- Delayed growth
- Passing small, watery, bloody stools
- Loss of energy.
Symptoms of Hirschsprung’s disease may resemble other conditions or medical problems. Please consult your child’s doctor for a diagnosis.
How is Hirschsprung’s disease diagnosed?
Our gastroenterologists perform a physical examination child, obtain a medical history and order a number of different tests in order to evaluate whether a child has Hirschsprung’s disease. These tests may include:
- Abdominal X-ray. A diagnostic test that may show a lack of stool in the large intestine or near the anus and dilated segments of the large and small intestine. Learn more about X-rays at CHOC.
- Barium enema. A procedure performed to examine the large intestine for abnormalities. A fluid called barium (a metallic, chemical, chalky, liquid used to coat the inside of organs so that they will show up on an X-ray) is given into the rectum as an enema. An X-ray of the abdomen shows strictures (narrowed areas), obstructions (blockages), and dilated intestine above the obstruction.
- Anorectal manometry. A test that measures nerve reflexes which are missing in Hirschsprung’s disease.
- Biopsy of the rectum or large intestine. A test that takes a sample of the cells in the rectum or large intestine and then looks for nerve cells under a microscope.
What is the treatment for Hirschsprung’s disease?
Specific treatment for Hirschsprung’s disease will be determined by your child’s doctor based on the following:
- The extent of the problem
- The child’s age, overall health and medical history
- The child’s tolerance for specific medications, procedures, or therapies
- Expectations for the course of the disorder
- The opinion of the health care providers involved in the child’s care
- The family’s opinion and preference.
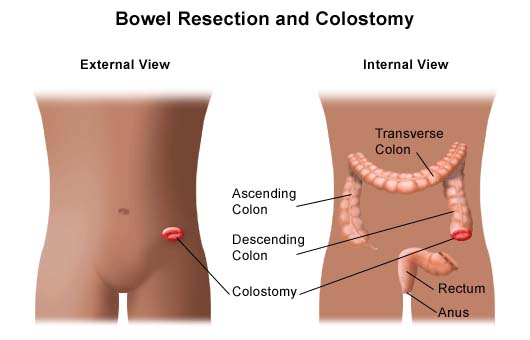
An operation is usually necessary to deal with intestinal obstruction caused by Hirschsprung’s disease. The surgeon removes the portion of the rectum and intestine that lacks normal nerve cells. When possible, the remaining portion is then connected to the anal opening. This is known as a pull-through procedure. At times, a child may need to have a colostomy done so stool can leave the body. With a colostomy, the upper end of the intestine is brought through an opening in the abdomen known as a stoma. Stool will pass through the opening and then into a collection bag. The colostomy may be temporary or permanent, depending on the amount of intestine that needs to be removed. After a healing period, many children can have the intestine surgically reconnected to the anal opening and have the colostomy closed.
Will my child have problems in the future?
Problems in the future often depend on the amount of intestine that lacked nerve cells, and how much intestine was removed. Children who are able to have their colostomy closed may have temporary or intermittent problems, including the following:
- Stools may be frequent and loose at first. Cleaning the anal area carefully to remove stool, and applying diaper rash creams or lotions may prevent skin irritation.
- Children may have problems sensing the need to have a bowel movement. Since the urge to have a bowel movement is greater after eating, setting aside 10 minutes after meals to spend on the toilet may help.
- Some children have problems with bowel movements because the anal opening is tight, and this can be helped by a special technique called rectal dilation. Your child’s doctor can teach you this technique if it is appropriate for your child.
Children who had a large section of intestine removed may have long-term problems. When a large portion of the intestine is removed, the digestive process can be affected. Nutrients and fluids are absorbed from food in the small intestine. Removing a large segment of the intestine can prevent a child from getting enough nutrients and fluids. Children can have problems with improper digestion, slow growth, and infection.
Consult your child’s doctor to talk about your child’s outlook.