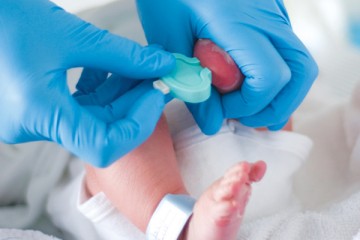
Precision Medicine and Pediatric Cancer Treatment
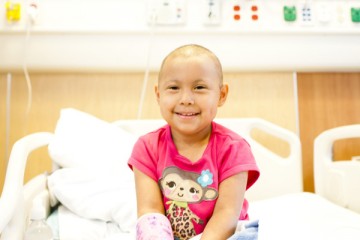 Until recently, precision medicine – personalized medicine using genetics and a patient’s health information to design a targeted treatment for a person’s specific disease – seemed like science fiction. Today, new technologies, more affordable human genome sequencing and advanced computer capabilities have made this a reality.
Until recently, precision medicine – personalized medicine using genetics and a patient’s health information to design a targeted treatment for a person’s specific disease – seemed like science fiction. Today, new technologies, more affordable human genome sequencing and advanced computer capabilities have made this a reality.
In 2015, President Obama announced the launch of the Precision Medicine Initiative to accelerate a new era of medicine that delivers the right treatment at the right time to the right person, taking into account individuals’ health history, genes, environments, and lifestyles. Then in 2016, the White House announced the Cancer Moonshot Task Force to lead a new, national initiative to eliminate cancer as we know it using precision medicine.
Precision medicine refers to the tailoring of medical treatment to the individual genetic characteristics of each patient’s disease. It does not literally mean creating special drugs or medical devices that are unique only to that patient. However, it may mean creating a unique combination of treatment modalities, including immunotherapy specifically designed for each patient.
While there is promise for the treatment of many types of diseases, including metabolic and neurodegenerative disorders, precision medicine has had its earliest success in cancer research and therapies, especially pediatric cancers.
Precision Medicine and Pediatric Cancer
For more than a decade, the cure rate for pediatric cancer has been stalled at about 80 percent. Experts are hoping to use precision medicine and genomic profiling to target and cure the other 20 percent. Genomic profiling is a laboratory method that is used to learn about all the genes in a person or in a specific cell type, and the way those genes interact with each other and with the environment.
Genomic profiling of cancer tumors will allow the pediatric cancer community to target, understand and individualize cancer treatment, with a goal of the least toxicity by harnessing a patient’s own immune system and using the tumor’s unique genomic mutations to create individual cancer vaccines.
In recent years, tumor profiling has become a valuable tool for oncologists when making treatment decisions for patients with recurrent (relapsed), or difficult‐to‐treat (refractory), rare and aggressive childhood cancers. By decoding genomic data from a tumor, and combining that information with a clinical strategy to optimize the immune system, we can provide personalized information to aid new treatment options.
Knowledge is the best medicine. Learn more about your child's health in these features from the experts at CHOC.
The Truth About Genetics
Medical genetics involves the study of inherited diseases. The field includes genetic counseling and testing, and their application to patient care in the practice of medicine.
Metabolic Tests at Birth
Metabolic tests are done on newborns with very small blood samples that are taken at birth from every baby in California.
Treating the Teen Cancer Patient
Teen cancer patients face unique challenges when dealing with cancer. Doctors need to take into account self-esteem, body issues, and emerging independence.